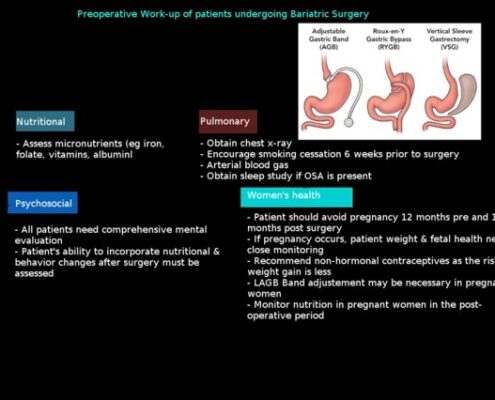
Gastric Sleeve
In sleeve gastrectomy, the equivalent of 75 to 80% of the stomach is removed … and it is the most frequently performed operation in the world to lose weight ..
Sleeve gastrectomy has profound effects in life:
overall improvement in the quality of life
In which the equivalent of 60-70% of weight gain is lost during the first year of the operation
Cure or improve obesity-related health diseases such as type 2 diabetes, high blood pressure, and stop
Sleep apnea, fatty liver, joint pain and hyperlipidemia.
Decreased appetite to eat food.
Decreased sense of hunger
What are the effects of sleeve gastrectomy:
A stomach size reduction is performed, so people feel full sooner after the operation.
Make people feel less hungry (ghrelin) – hormonal changes such as those related to a lack of secretion of hunger hormones
– The increase in gastric motility makes food pass through the stomach and intestine faster.
History and Trend of the Gastric Sleeve
Initially, the Gastric Sleeve was the restrictive part of the biliopancreatic diversion duodenal switch operation. Then, the gastric sleeve became the first stage operation for very obese patients who underwent duodenal switch operation to reduce the perioperative risks. Some patients lost enough weight after the gastric sleeve surgery and did not undergo the planned second stage duodenal switch operation. These findings prompted bariatric surgeons to consider the gastric sleeve surgery as a standalone bariatric procedure. The first laparoscopic Gastric Sleeve was performed in 2000.
Over the past decade, the number of gastric sleeve surgeries continue to increase nearly every year. Now, more than half of all bariatric surgeries performed in US are gastric sleeve procedures.
How much weight will I lose after the Gastric Sleeve?
On average, people lose about 60-70% of their excess weight
The first 2 weeks: 10-20 pounds; most patients lose about one pound a day
The first 3 months: 35-45% of excess weight loss
The first 6 months: 50-60% of excess weight loss
The first year: 60-70% of excess weight loss
Most people reach their lowest weight 12-24 months after surgery
The Gastric Sleeve success rate is approximately 80-90%
Improvement of Obesity Related Health Problems
Large clinical trials and studies have proven gastric sleeve surgery lead to resolution or improvement of many obesity related health problems such as:
Type 2 diabetes: Most studies indicated that 60-80% of patients with type 2 diabetes could achieve disease remission or improvement after gastric sleeve surgery
- Hypertension
- Fatty liver disease
- High cholesterol
- Sleep apnea
- Decreased cancer risk
- PCOS
- Asthma
- Migraine
- Join pain
- Depression and other psychosocial problems
- Infertility
- Low testosterone: Gastric sleeve can naturally lead to increased testosterone level
- Urinary incontinence
- Gout
According to the SAGES (Society of American Gastrointestinal and Endoscopic Surgeons) guidelines for bariatric surgery, the indications for weight loss surgery are as follows:
BMI more than 40 without comorbidities
BMI 35 to 39.9 with at least one serious comorbidity including diabetes, hypertension, sleep apnea or limitations in the quality of life
BMI 30 to 34.9 with metabolic syndrome or diabetes that is uncontrolled with medical therapy
It is important to note that upon entrance to a bariatric surgery program and before proceeding with surgery, patients should participate in a guided weight loss program with exercise and lifestyle modifications; this will help ensure that the patient can make the commitment necessary to undergo the postoperative nutritional restrictions of the procedure.
A BMI of 20 to 25 kg/m2 identifies a subject with a normal weight, whereas a BMI of 26 to 29.9 kg/m2 is considered overweight, and a BMI of 30 to 39.9 kg/m2 is considered obese. A patient with a BMI over 40 kg/m2 is called extremely obese; a patient with a BMI over 50 kg/m2 is superobese, and with a BMI greater than 60 kg/m2 is super-super obese.
Recovery after Surgery
The surgery takes approximately 40-70 minutes
Discharge from hospital typically occurs after 1-2 nights
All patients are encouraged to walk as early as 3-4 hours after surgery
In general, the pain is easily manageable after surgery. Most patients take less than the recommended pain medication
Most patients go back to work and/or school after 2-4 weeks. Fatigue is common the first 2 weeks due to low calorie intake from liquid diet. However, the majority of patients do not feel hungry during this stage of the diet. The energy level improves quickly after the introduction of the soft diet, which is approximately 2 weeks after surgery. On occasion, we allow patients to work from home 2-3 days per week after surgery.
Patients can begin exercising 4 weeks after surgery
Complications and Risks
Over the past decade, with the improvement of surgical techniques and surgeons’ experience, the gastric sleeve has become an overall safe bariatric surgical procedure. However, complications can still occur during and after surgery. Below are the main complications and risks of the gastric sleeve surgery:
Leakage from the staple line – this is a rate but serious complication of the gastric sleeve surgery. The reported leak rate is between 0.7-3 percent. At UCLA, we pay paramount attention to our surgical techniques to minimize all the complications. At this point, we have never had a leak from the gastric sleeve surgery at UCLA.
Stricture/stenosis – In the past, we had one stricture among our first 20 gastric sleeve procedures. We have not had any strictures within the past 5 years.
Bleeding
Blood Clot
Heart Burn – This is a very controversial topic in bariatric surgery and the data from different centers is inconsistent. In our experience, most patients with heartburn before surgery see improvement of symptoms after surgery due to weight loss. Some patients may develop new heartburn, which is treatable with over-the-counter anti-acid medications, in most cases.
Nutrient or vitamin deficiency
Weight Regain – After 1-2 years, slight weight regain is common among all bariatric procedures and about 10-20% of patients can have significant weight regain after gastric sleeve surgery. After 5 years of follow up, many centers collected data to show that the majority of patients can maintain their weight loss after the Gastric Sleeve Surgery.
Excess skin due to rapid weight loss in a short period.
Nutrition after the sleeve gastrectomy
After the operation of the sleeve gastrectomy, the patient needs a special diet for a period of thirty-five days, and this diet is divided according to time into several patterns or stages, which are the clear liquids phase for a period of ten days, the phase of full fluids and pureed foods for another ten days, then the phase of soft meals for ten days, and finally Back to the natural food system, and at each stage there are specific types of foods that are allowed to be consumed.
The first day: to follow a liquid diet. Some surgeons allow patients to drink water a few hours after surgery
Clear fluid phase (10-14 days)
The patient can drink at this stage liquid soups such as broth, apple juice or filtered carrot juice without drinking citrus juice, and herbs such as flowers, anise or chamomile can be drunk, in addition to water, tea and coffee.
Full Fluid Phase (10 days)
This stage contains pure or thick soups mashed in a blender, such as vegetable soup, lentils, vermicelli, etc., and watermelon, melon or carrot juice can be drunk, and yogurt and low-fat milk are consumed, in addition to other liquids.
Pureed Food Stage (10 days)
The patient can, at this stage, eat any type of liquid present in the previous two stages, in addition to eating well-mashed fruits in an electric mixer, as well as drinking fruit cocktails, grilled or boiled vegetables that must be mashed, or eating starches such as rice soup or breakfast cereals with milk low fat. At this stage, it is forbidden to eat meat from fish or white and red meat, as well as eating bread and all kinds of soft drinks like Pepsi and coca cola , for a period of three to six months after the operation.
The normal diet phase after 30-34 days
It is possible to return to eating various foods and eating meat and solid foods, and at this stage the next tips must be followed to avoid any stomach imbalance: Eat slowly and chew well. Refrain from eating as soon as you feel full. Not to eat and drink at the same time. Distribute food to different times and eat six to eight snacks.
After surgery, all patients should take multi-vitamin and B complex
Exercise after the sleeve gastrectomy
Be careful not to neglect the sport after the operation; In addition to diet, exercise helps to lose weight in a healthy way, and the intensity of exercise must be gradually increased after the sleeve, where the patient begins to walk for a period of half an hour or more, then after a week he starts swimming, then after a month it is possible to ride a bicycle, and after three months he begins With stomach-tightening exercises and aerobics.
Comparison of Gastric Sleeve to other Types of Bariatric Procedures
Laparoscopic gastric banding (Lap-band) was once very popular. However, due to its high rate of long term complications and inferior weight loss, the number of Lap-band surgeries went down every year in the US and worldwide. Most of the US large academic Bariatric Surgery Centers rarely perform the Lap-band procedure at this time.
Laparoscopic Roux-en-Y Gastric Bypass Surgery is the gold standard of bariatric surgery. However, Gastric Sleeve has replaced the Gastric Bypass Surgery as the most popular bariatric surgery in recent years due to its technical simplicity and fewer long-term complication rates.
Advantage of Gastric Sleeve versus Gastric Bypass Surgery
Technically, the Gastric Sleeve is a much simpler surgery. The operating time for gastric sleeve is usually 40-70 minutes, while gastric bypass surgery takes approximately 2-3 hours to complete.
There is a much lower chance for nutrient or vitamin deficiency with the Gastric Sleeve procedure. In addition, there is no mal-absorption for Gastric Sleeve patients.
Some long-term complications could occur with the Gastric Bypass patients including bowel obstruction, marginal ulcer, and internal hernias. The chance of Gastric Sleeve patients developing these complications is exceedingly rare.
Preoperative Imaging
There is no consensus regarding the imaging modalities that should be obtained before a bariatric procedure
An abdominal ultrasound is necessary for patients undergoing gastric bypass to identify possible liver pathology and cholelithiasis due to the high prevalence of the latter in this patient population.
patients with symptoms of acute or chronic cholecystitis or symptomatic cholecystitis should have their gallbladder removed during the bariatric procedure, as weight loss will only worsen their symptoms.
Esophagogastroduodenoscopy (EGD) is not routinely a recommended procedure in the workup for bariatric surgery. The American Society of Metabolic and Bariatric Surgery advises the use of endoscopy only for patients with significant gastrointestinal symptoms.
What are the routine tests before surgery?
Certain basic tests are done prior to surgery:
- A complete blood count
- Urinalysis
- Chemistry panel
- Gallbladder ultrasound
- The chemistry panel gives results of about 20 blood chemistry values. Many surgeons also ask for a gallbladder ultrasound to look for gallstones.
Other tests may be requested when indicated and include:
- Chest X-ray
- Electrocardiogram
- Pulmonary function testing
- Echocardiogram
- Sleep studies
- GI evaluation
- Cardiology evaluation
- Psychiatric evaluation
The Comprehensive Metabolic Panel CMP includes the following tests:
Calcium
Albumin
Total Protein
*Electrolytes:
Sodium
Potassium
*Kidney Tests
Blood urea nitrogen (BUN)
Creatinine
Alkaline phosphatase (ALP)
Liver Tests
Alanine amino transferase (ALT,) –
Aspartate amino transferase (AST,)
Bilirubin.
Blood Test
Hemoglobin
Lipid Profile
TFT
What is the purpose of pre-operative bariatric surgery tests?
An accurate assessment of your health is needed before surgery. The best way to avoid complications is to understand their potential in the first place. It is important to know if your thyroid function is adequate since hypothyroidism can lead to sudden death post-operatively.
If you are diabetic, special steps must be taken to control your blood sugar. Because surgery increases cardiac stress, your heart will be thoroughly evaluated.
These tests will determine if you have:
- Liver malfunction
- Breathing difficulties
- Excess fluid in the tissues
- Abnormalities of the salts or minerals in body fluids
- Abnormal blood fat levels
Why is a gastrointestinal evaluation necessary?
Patients with significant gastrointestinal symptoms such as:
- Upper abdominal pain
- Heartburn
- Belching
- Sour fluid
They may be symptomatic of underlying problems including:
- Hiatal hernia
- Gastroesophageal reflux and/or
- Peptic ulcer
- Up to 15 percent of reflux patients may show early damage in the lining of the esophagus, which could predispose them to cancer of the esophagus. It is important to identify this so a suitable surveillance or treatment program can be planned.
Why must I complete a sleep study?
The sleep study detects a tendency for sleep apnea. The abnormal stopping of breathing usually associated with airway blockage when the muscles relax during slumber. This condition is associated with a high mortality rate.
Sleeping after bariatric surgery
After surgery you will be sedated and will receive pain narcotics, which further depress normal breathing and reflexes. Airway blockage also becomes more dangerous at this time. It’s important that your surgeon has clear expectations of the procedure so he can decide how to handle possible irregularities.
What impact do medical problems have on bariatric surgery?
Medical problems such as serious heart or lung problems can increase the risk of any surgery. Conversely, if these problems are related to the patient’s weight, they also increase the need for surgery. Severe medical problems may not dissuade the surgeon from recommending bariatric surgery if it is otherwise appropriate, but those conditions will make a patient’s risk higher than average.
Contraindications
There are several contraindications for bariatric surgery procedures which include:
Major depression or uncontrolled mental health problem
Current substance misuse, including alcoholism
Patients determined to be non-compliant with nutritional requirements and supplementation after bariatric surgery
Underlying eating disorders
Severe coagulopathies
Patient-related contraindications to undergo surgery (cardiovascular risk, anesthetic risk)
A relative contraindication to sleeve gastrectomy procedure is gastroesophageal reflux disease which can become significantly worse after a sleeve gastrectomy
Points to be addressed for Gastric Sleeve and Pregnancy
Follow up Visits after surgery and labs required:
The American Society for Metabolic & Bariatric Surgery (ASMBS) guidelines for postsurgical tests following bariatric procedures in the USA have remained unchanged for the last decade.
The ASMBS guidelines recommend postoperative blood testing every 3 months for the first year, every 6 months for the second year, and annually thereafter regardless of the type of bariatric procedure performed.
other bariatric guidelines (other than USA) recommend less frequent postoperative lab testing.
We usually ask on routine follow up visits for:
CBC, KFT, LFT, TSH, Lipid profile, Zinc, Mg, Ca, Vit B12, Vit D, Uric acid, Folic acid, Iron, Ferritin and HbA1c.
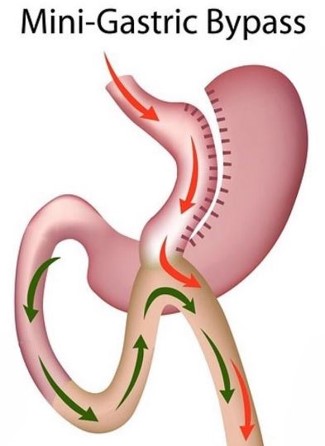
Mini Gastric Bypass (MGB)
A gastric bypass is a surgical procedure to treat obesity that involves reducing the size of your stomach to facilitate early satiety and bypassing a section of your intestine to limit food absorption. As with the sleeve procedure, a reduction in size of the stomach restricts the amount of food intake and appetite.
Procedure Mini gastric bypass, One anastomosis gastric bypass
This procedure was traditionally carried out by a Roux-Y procedure where stomach and intestine are reconnected in two places. A single anastomosis gastric bypass is a modification that simplifies this procedure, reducing operating time and complications both early and late.
EXPECTED WEIGHT LOSS
30-50% total body weight loss
SURGICAL PROCEDURE:
The gastric pouch is constructed similar to a sleeve gastrectomy but not as long. The small bowel is then measured 150-200 cm downstream and joined to the end of the gastric pouch.
ADVANTAGES
Laparoscopic procedure “keyhole surgery” so less invasive
Limits the amount of food ingested and also the calories absorbed
Increases intestinal production of GLP1 which stimulates insulin release and is more potent for diabetes cure
Ability to eat bread and meat is a little easier
A little more weight loss than sleeve
Potentially reversible
DISADVANTAGES
- Vitamin and trace element deficiency
- Intolerance to certain foods
- Dumping syndrome
- Requires a lifelong multivitamin
- Bile reflux, though rare
RECOMMENDED FOR PATIENTS WITH:
- High BMI >45
- Diabetics
- Severe reflux
- Prior gastric banding
- Patient preference
RECOVERY
After gastric bypass surgery:
- you will stay in hospital for 1 night and have an x-ray in the morning (gastrograffin meal)
- you will have pain relieving medications to keep you comfortable
- you will be given instructions to follow regarding wound care, diet and activity
- you will take Somac or Nexium for 3 months and then stop if reflux free
Patients should:
- Keep the incision area clean and dry
- Avoid strenuous exercises and lifting heavy weights for 2 weeks
- Sip water throughout the day to prevent dehydration
- Follow the diet regimen given to you by the dietitian
- Follow an exercise program to maintain weight loss
POSSIBLE COMPLICATIONS
- Lifelong follow up with a physician is required for blood tests to ensure proper health and nutrition
- Bowel leak through the anastomosis (surgical joins)
- Gallstones
- Dumping syndrome – meals flood the intestine causing dizziness, nausea and diarrhoea
- Nausea
- Dehydration
- Indigestion
- Reactive hypoglycaemia
- Nutrient deficiencies
- Incisional hernia
- Wound infections
- Marginal ulcers
- Stomal stenosis
- Haemorrhage
- Infection
- Bleeding
- Bile reflux
- Venous thromboembolism